by KAROLA KLATT
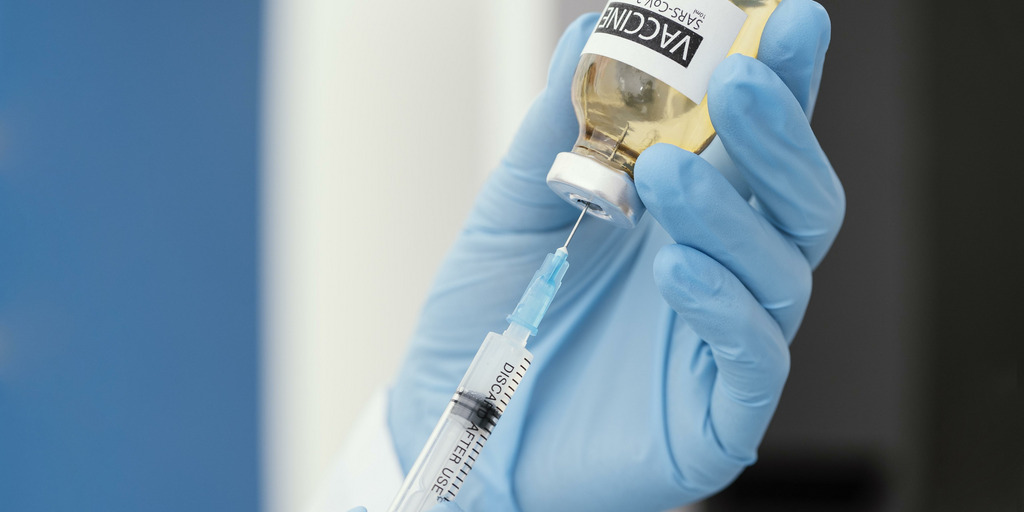
Fair access to health services and the fight against unhealthy living conditions are the focus of the World Health Organisation's campaign for World Health Day on 7 April, 2021. COVID-19 has highlighted how some people live healthier lives and enjoy better access to health services than others. The vaccine supply reflects this injustice: the pandemic is a global problem that can only be solved globally but national self-interest continues to dominate politics.
Moreover, injustice is not only international, but also evident within the health systems of many industrialised countries. Underfinanced and inefficient, many places have seen a shortage of care, resulting in long waiting times for necessary treatment. A kind of two-class medical system has emerged that clearly disadvantages those with low incomes and little social security. During the corona crisis, the privatisation of health services has reduced the ability of governments to allocate health resources where they are most needed. The discriminatory effects of health systems even become dangerous drivers of the pandemic.
Fear of treatment costs intensifies U.S. pandemic
The Bertelsmann Foundation's latest Social Justice Index, which examines health as one of six measures of social justice in 41 industrialised countries, states: “One observation made by many country experts is the rapid growth of private sector activity in health care, which undermines the principle of inclusive health care.”
A prime example of this is the United States, which maintains the most expensive healthcare system in the world. But the nation lacks a comprehensive health insurance and doctor and hospital bills are responsible for around 60 percent of private insolvencies. For fear of being bankrupted by illness, many people have delayed getting tested for the virus or seeking treatment, creating a perfect breeding ground for the pandemic.
Numerous studies in the U.S. show that Blacks and Latinos are at increased risk of contracting COVID-19, suffering severe symptoms and even dying. The Kaiser Family Foundation monitors data across states and finds that Black and Hispanic Americans are also disadvantaged in access to vaccination across the board, even though their risk of illness and death is significantly higher compared to the white majority.
Greece forces private doctors to provide COVID-19 treatment
The Sustainable Governance Indicators (SGI) of the Bertelsmann Foundation have been examining the policies and governance capabilities of OECD and EU countries for 15 years and also assess the extent to which national health policies enable high-quality health care that is both accessible and cost-efficient. Experts see serious deficiencies in this regard in a total of 13 countries, 11 of which are EU member states.
One of these countries is Greece, where an oversupply of private medical services has developed due to austerity policies. In a comparison of industrialised countries, Greece has the highest density of doctors and yet there is a shortage of general practitioners and, above all, nurses. The majority of the many specialists work in the private sector because, according to the SGI country experts, they lack incentives to work for the state health care system. The authors criticise: “A high volume of unrecorded and untaxed transactions between patients and doctors as well as a differential in healthcare access based on the purchasing power of households.”
How this plays out in a pandemic situation became clear in November 2020, when the Greek Ministry of Health felt compelled to temporarily nationalise two private clinics in Thessaloniki to admit COVID-19 patients, which they had previously refused to do for fear of damaging their image. Similarly, in the third coronavirus wave in March 2021, Health Minister Vassilis Kikilias announced that he would forcibly recruit private doctors to treat COVID-19 patients if necessary.
Hungary criminalises bribery in health care
Another health system that has serious equity problems, according to the SGI country experts, is Hungary's: "The Orbán governments have failed to tackle the widespread mismanagement and corruption in the health sector, the large debt burden held by hospitals, the discretionary refusal of services by medical staffers, and the increasing brain drain of doctors and nurses to other countries. Good quality services are available in the private sector, but only for a small share of society."
Despite such harsh assessments within the international context, Prime Minister Viktor Orbán always considered himself well equipped against the pandemic. In fact, the government made a lot of progress in the fight against the virus: gaining broad support, starting its own production of disinfectants, protective equipment, medical consumables and ventilators, building temporary hospitals for COVID-19 patients and, as part of Orbán's "pragmatic foreign policy", purchasing Russian and Chinese vaccines, despite pending EU approvals.
The extent to which the Hungarian health system is nonetheless under pressure can be seen in a law that has just come into force: Since 1 March, health care workers face a three-year prison sentence if they accept “thank-you” money. And patients can also be sentenced to prison for offering bribes.
Germany has also experienced cases of people profiting from their connections, in terms of vaccinations and pandemic shortages. The numerous studies on disadvantaged populations make it clear that the fight against COVID-19 is a justice issue internationally as well as within national borders. Giving privileged people preferential treatment and access to vaccinations contradicts democratic values of equality for all citizens. Even in the richest countries of the world, governments must ensure equity infuses all aspects of their pandemic response. This is essential to ensure that public trust in their political systems is not squandered.
Karola Klatt is a science journalist and editor of SGI News and the Bertelsmann Stiftung's BTI blog.
Translated from the German by Jess Smee
A version of this article was first published on Social Europe